Hidradenitis suppurativa is a chronic inflammatory skin condition that causes painful lumps under the skin. Understanding its causes, symptoms, and treatments can help you manage it effectively and improve daily life.
Hidradenitis suppurativa (HS) is often misunderstood and frequently misdiagnosed. Many people initially think the condition is simply recurring boils or acne, but it is actually a long-term inflammatory disease that affects the hair follicles and sweat glands. HS typically appears in areas where skin rubs together, such as the armpits, groin, inner thighs, and under the breasts.
Learning more about hidradenitis suppurativa can empower you to recognize symptoms early, explore treatment options, and adopt lifestyle changes that reduce flare-ups. In this guide, you’ll discover what causes HS, how it develops, and which treatments may help you manage the condition more effectively.
What Is Hidradenitis Suppurativa and Why Does It Develop?
Hidradenitis suppurativa is a chronic inflammatory skin disease that develops when hair follicles become blocked and inflamed. This blockage leads to painful nodules, abscesses, and sometimes tunnels under the skin called sinus tracts.
Although the exact cause of HS is not fully understood, research suggests that the condition involves a combination of immune system dysfunction, genetics, and environmental factors.
How the Condition Begins
The process usually starts with clogged hair follicles. When these follicles rupture beneath the skin, the body triggers an inflammatory response. This inflammation leads to the formation of painful lumps and abscesses.
Over time, repeated inflammation may cause:
- Thickened skin
- Scarring
- Interconnected tunnels under the skin
- Chronic drainage from lesions
HS is not contagious and is not caused by poor hygiene, though many people mistakenly believe otherwise.
Who Is Most at Risk?
Certain groups are more likely to develop hidradenitis suppurativa. Risk factors include:
- Family history of HS
- Hormonal influences
- Smoking
- Obesity
- Age between puberty and 40 years
Women are generally affected more frequently than men.
What Are the Most Common Symptoms of Hidradenitis Suppurativa?
The symptoms of hidradenitis suppurativa often begin subtly but may worsen over time if untreated. Early recognition can significantly improve management.
Early Signs
In its earliest stage, HS may appear as small tender bumps that resemble pimples or ingrown hairs. These bumps typically occur in areas with friction or sweat.
Common early symptoms include:
- Small painful lumps under the skin
- Blackhead-like spots in clusters
- Redness and swelling
- Warm, tender areas on the skin
These lesions may persist for weeks or months.
Advanced Symptoms
As the disease progresses, symptoms can become more severe.
These may include:
- Large painful abscesses
- Recurrent flare-ups in the same area
- Thick scars or rope-like skin texture
- Draining lesions with an unpleasant odor
- Formation of sinus tracts beneath the skin
Because HS can be painful and persistent, it can also affect emotional well-being and quality of life.
How Is Hidradenitis Suppurativa Diagnosed?
Diagnosing hidradenitis suppurativa can sometimes be challenging because the symptoms resemble other skin conditions.
Dermatologists usually rely on three key criteria:
- Typical lesions such as nodules, abscesses, or sinus tracts
- Characteristic locations like armpits, groin, buttocks, or under the breasts
- Recurrent episodes of lesions in the same areas
Medical Evaluation
A healthcare provider may perform:
- A detailed skin examination
- Review of medical history
- Assessment of symptom patterns
Laboratory tests are rarely needed but may help rule out infections or other inflammatory diseases.
Disease Staging
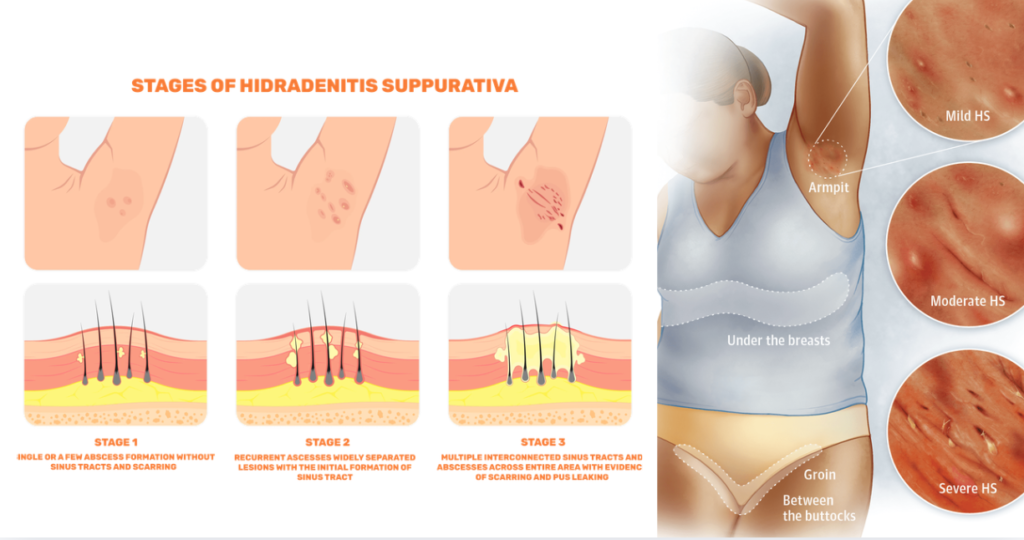
Doctors often classify HS using the Hurley staging system:
- Stage 1: Single or multiple abscesses without scarring
- Stage 2: Recurrent abscesses with sinus tracts and scarring
- Stage 3: Extensive interconnected tunnels and widespread inflammation
The stage helps determine the most appropriate treatment strategy.
What Treatment Options Are Available for Hidradenitis Suppurativa?
Although hidradenitis suppurativa cannot currently be cured, several treatments can significantly reduce symptoms and prevent complications.
Treatment usually focuses on controlling inflammation, preventing new lesions, and managing pain.
Medical Treatments
Doctors may prescribe medications depending on disease severity.
Common options include:
Topical treatments
- Antibiotic creams such as clindamycin
- Anti-inflammatory agents
Oral medications
- Antibiotics to reduce inflammation and bacteria
- Hormonal therapy in some patients
- Retinoids for certain cases
Biologic therapies
Newer medications that target immune pathways have shown promising results for moderate to severe HS.
These treatments help regulate the immune system and reduce chronic inflammation.
Surgical Procedures
When lesions become persistent or severe, surgical options may be considered.
These may include:
- Drainage of painful abscesses
- Removal of sinus tracts
- Wide surgical excision of affected areas
Surgery may help prevent repeated flare-ups in specific regions.
What Lifestyle Changes Can Help Manage HS Symptoms?
While medical treatment is essential, lifestyle adjustments can play a major role in managing hidradenitis suppurativa.
Weight Management
Studies show that excess body weight may worsen HS symptoms. Losing weight can reduce skin friction and inflammation.
Smoking Cessation
Smoking is strongly linked to HS severity. Quitting smoking may decrease flare frequency and improve treatment outcomes.
Skin Care Practices
Gentle skin care can help reduce irritation.
Helpful strategies include:
- Wearing loose clothing
- Using mild antibacterial cleansers
- Avoiding harsh shaving methods
- Keeping affected areas clean and dry
These steps can reduce friction and minimize irritation.
What Complications Can Occur If HS Is Left Untreated?
Without proper management, hidradenitis suppurativa can lead to several complications.
Physical Complications
Chronic inflammation may cause:
- Permanent scarring
- Restricted movement due to thick scar tissue
- Secondary infections
- Lymphedema (swelling caused by blocked lymphatic drainage)
In rare cases, long-standing HS may increase the risk of certain skin cancers.
Emotional and Psychological Impact
Living with a chronic skin condition can affect mental health.
Some individuals experience:
- Social anxiety
- Depression
- Reduced self-confidence
- Difficulty with daily activities
Support groups, counseling, and medical care can help address these challenges.
How Can You Prevent HS Flare-Ups?
Although flare-ups cannot always be avoided, several strategies can reduce their frequency and severity.
Preventive steps include:
- Maintaining a healthy weight
- Avoiding tight clothing that causes friction
- Managing stress levels
- Following prescribed treatment plans
- Identifying personal triggers such as heat or certain skincare products
Tracking symptoms and triggers may also help you recognize patterns and adjust your routine accordingly.
Maximizing Long-Term Management and Living Well With HS
Managing hidradenitis suppurativa is a long-term process that often requires a combination of medical care and lifestyle adjustments.
You can improve your quality of life by:
- Building a strong relationship with a dermatologist
- Following treatment plans consistently
- Seeking support from patient communities
- Staying informed about new research and therapies
Emerging treatments and ongoing research continue to improve outcomes for individuals living with HS.
Conclusion
Hidradenitis suppurativa is a complex chronic skin condition that can significantly impact daily life, but understanding the disease is the first step toward effective management. By recognizing the symptoms early, exploring medical treatments, and adopting supportive lifestyle habits, you can reduce flare-ups and regain control over your skin health.
If you suspect you may have hidradenitis suppurativa, seeking professional medical guidance can help you develop a personalized treatment plan. With the right combination of care, knowledge, and support, living well with HS is entirely achievable.
Important Disclaimer: This article is for informational purposes only and should not replace professional advice. For health-related topics, consult healthcare providers. For financial or legal matters, seek qualified professional guidance. For safety procedures, verify current best practices and local regulations. Individual results may vary, and personal circumstances should always be considered when implementing any suggestions.