Minerals constitute inorganic micronutrients essential for virtually every physiological process in the human body, from enzymatic catalysis to structural integrity of tissues. Unlike macronutrients that provide energy, minerals function as cofactors, electrolytes, and structural components that enable biochemical reactions fundamental to life. Understanding which minerals your body requires, their specific physiological roles, and optimal dietary sources empowers you to make informed nutritional decisions that support long-term health outcomes and prevent deficiency-related pathologies.
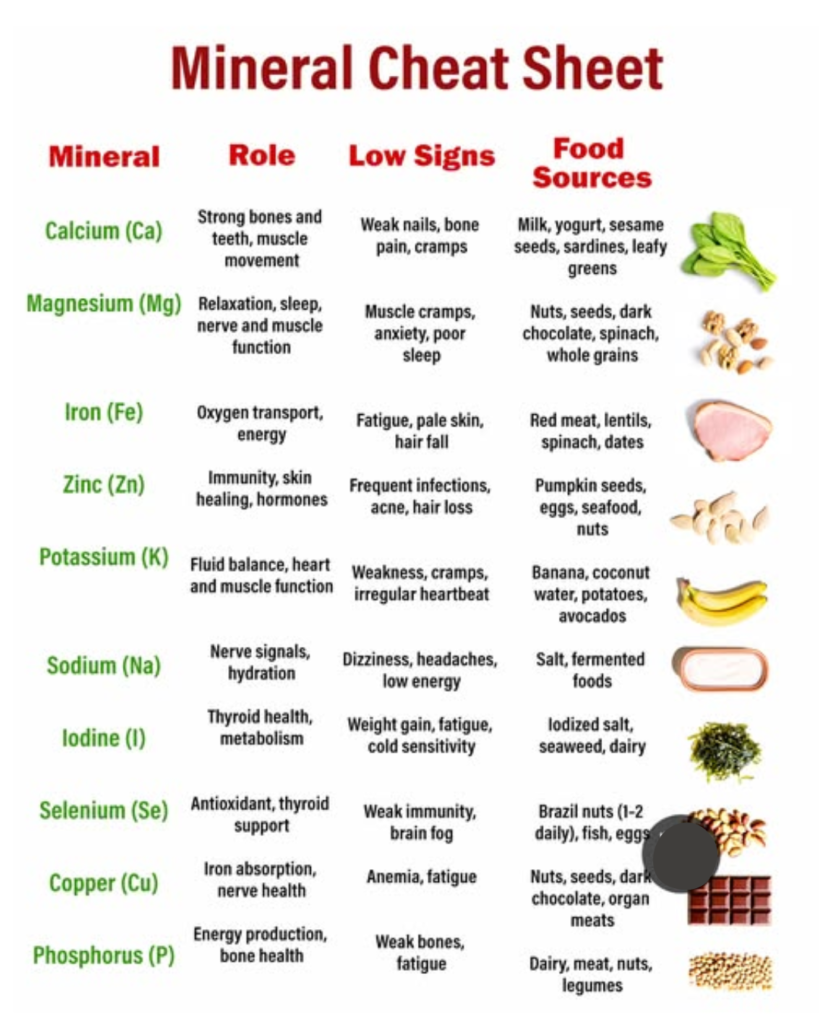
Understanding Mineral Classification and Bioavailability
Before examining specific minerals, it’s important to understand how nutritional science categorizes these nutrients and the factors affecting their absorption and utilization.
Major Minerals Versus Trace Elements
Minerals are classified based on the quantity required by the human body. Major minerals (macrominerals) are needed in amounts exceeding 100 milligrams daily and include calcium, phosphorus, magnesium, sodium, potassium, chloride, and sulfur. Trace elements (microminerals) are required in smaller quantities—typically measured in micrograms or low milligrams—but remain equally essential for physiological function. These include iron, zinc, copper, selenium, iodine, manganese, fluoride, chromium, and molybdenum.
This quantitative distinction doesn’t reflect relative importance—trace elements perform functions that cannot be fulfilled by major minerals. Rather, the classification reflects evolutionary metabolic requirements and the prevalence of these elements in ancestral dietary environments.
Factors Influencing Mineral Absorption
Mineral bioavailability—the proportion of ingested mineral that enters systemic circulation and becomes available for physiological use—varies substantially based on chemical form, concurrent dietary components, and individual physiological status. Minerals bound in organic complexes (such as heme iron in meat) typically exhibit higher bioavailability than inorganic salts. Certain dietary factors enhance absorption: vitamin C increases non-heme iron absorption, while vitamin D facilitates calcium uptake.
Conversely, absorption inhibitors include phytates (found in grains and legumes), oxalates (in spinach and certain vegetables), and polyphenols (in tea and coffee), which form insoluble complexes with minerals. Additionally, minerals can compete for shared absorption pathways—excessive zinc intake impairs copper absorption, while high calcium consumption reduces iron and magnesium uptake. Understanding these interactions enables optimization of mineral status through strategic dietary composition.
The Ten Essential Minerals: Physiological Roles and Health Implications
The following minerals represent those with the most extensively documented roles in human health, supported by substantial biochemical and clinical evidence.
Calcium: Skeletal Structure and Cellular Signaling
Calcium serves dual critical functions: providing structural integrity to bones and teeth (containing 99% of body calcium) while functioning as a ubiquitous intracellular signaling molecule. Bone tissue exists in dynamic equilibrium with plasma calcium through continuous remodeling—osteoblasts deposit calcium in hydroxyapatite crystals while osteoclasts resorb bone to maintain serum calcium homeostasis. This homeostatic regulation, controlled primarily by parathyroid hormone and calcitonin, prioritizes plasma calcium levels even at the expense of skeletal stores.
Beyond structural roles, calcium ions mediate neurotransmitter release, muscle contraction (both skeletal and cardiac), blood coagulation cascades, and numerous enzymatic reactions. Intracellular calcium concentration fluctuations serve as signals triggering specific cellular responses, making calcium homeostasis critical for normal physiology.
Recommended Intake: Adults require approximately 1,000-1,200 mg daily, with requirements increasing during adolescence, pregnancy, and post-menopausal years due to accelerated bone turnover.
Optimal Sources: Dairy products provide highly bioavailable calcium (250-300 mg per cup of milk). Non-dairy sources include fortified plant milks, sardines with bones (325 mg per 3-ounce serving), calcium-set tofu (200-400 mg per serving), and certain leafy greens like kale and bok choy—though oxalate content in spinach significantly reduces calcium bioavailability despite high total content.
Iron: Oxygen Transport and Enzymatic Function
Iron’s primary function involves oxygen transport via hemoglobin (in erythrocytes) and myoglobin (in muscle tissue), accounting for approximately 70% of body iron. Each hemoglobin molecule contains four iron atoms that reversibly bind oxygen, enabling efficient oxygen delivery from pulmonary capillaries to peripheral tissues. Beyond oxygen transport, iron serves as a cofactor for cytochromes in the electron transport chain (enabling cellular respiration), catalase and peroxidase enzymes (protecting against oxidative stress), and ribonucleotide reductase (essential for DNA synthesis).
Iron deficiency represents the most prevalent nutritional deficiency globally, affecting approximately 1.6 billion people. Progressive deficiency manifests initially as depleted iron stores (ferritin), then iron-deficient erythropoiesis, and finally iron deficiency anemia characterized by microcytic, hypochromic red blood cells, fatigue, impaired cognitive function, and compromised immune response.
Recommended Intake: Males require approximately 8 mg daily, while premenopausal females need 18 mg due to menstrual blood loss. Pregnancy demands increase to 27 mg daily to support expanded maternal blood volume and fetal development.
Optimal Sources: Heme iron from animal tissues (red meat, poultry, fish) exhibits 15-35% bioavailability compared to 2-20% for non-heme iron from plant sources. Beef liver provides exceptional iron density (5 mg per 3-ounce serving). Plant sources include lentils (3.3 mg per cup), fortified cereals (variable, up to 18 mg per serving), and spinach (though absorption is limited by oxalates). Consuming vitamin C with plant iron sources significantly enhances absorption through reduction of ferric (Fe³⁺) to ferrous (Fe²⁺) iron.
Magnesium: Enzymatic Cofactor and Neuromuscular Function
Magnesium participates as a cofactor in over 300 enzymatic reactions, including those involved in ATP synthesis, DNA/RNA synthesis, protein synthesis, and glucose metabolism. Approximately 60% of body magnesium resides in bone tissue, serving as a reservoir for maintaining extracellular concentrations. The remaining magnesium distributes between intracellular compartments (where it stabilizes ATP and nucleic acid structures) and extracellular fluid (where it influences neuromuscular excitability and cardiovascular function).
Magnesium modulates ion channels, particularly calcium channels, thereby influencing muscle contraction, nerve transmission, and cardiac rhythm. It also functions in parathyroid hormone secretion and vitamin D metabolism, creating interdependence among these nutrient systems. Chronic suboptimal magnesium status—present in an estimated 50% of Western populations—associates with increased risk of type 2 diabetes, hypertension, osteoporosis, and cardiovascular disease, though causality remains debated.
Recommended Intake: Adult males require 400-420 mg daily, while females need 310-320 mg, with increases during pregnancy to 350-360 mg.
Optimal Sources: Green leafy vegetables provide magnesium through the central magnesium atom in chlorophyll molecules—spinach offers 157 mg per cooked cup. Nuts (almonds: 80 mg per ounce), seeds (pumpkin seeds: 150 mg per ounce), whole grains (brown rice: 84 mg per cup), and legumes (black beans: 120 mg per cup) represent excellent sources. Dark chocolate provides 64 mg per ounce, illustrating that nutrient density exists across diverse food categories.
Zinc: Immune Function and Protein Synthesis
Zinc serves structural, catalytic, and regulatory roles across hundreds of enzymes (estimates range from 300-3,000 zinc-dependent proteins). It functions in DNA synthesis and repair, protein synthesis, cell division, immune function, wound healing, and sensory perception (taste and smell). Zinc finger motifs—protein structural domains coordinated by zinc ions—enable transcription factor binding to DNA, regulating gene expression throughout the genome.
Immunologically, zinc influences both innate and adaptive immunity through multiple mechanisms: maintaining epithelial barrier integrity, supporting neutrophil and natural killer cell function, regulating T-lymphocyte development and function, and modulating cytokine production. Zinc deficiency impairs these processes, manifesting as increased susceptibility to infections, delayed wound healing, and in severe cases, growth retardation and hypogonadism.
Recommended Intake: Adult males require 11 mg daily, while females need 8 mg, increasing to 11-12 mg during pregnancy and lactation.
Optimal Sources: Oysters provide exceptional zinc concentration (74 mg per 3-ounce serving)—far exceeding other sources. More practical sources include beef (7 mg per 3-ounce serving), crab (6.5 mg per 3 ounces), fortified cereals (variable), pumpkin seeds (2.2 mg per ounce), and chickpeas (2.5 mg per cup). Animal sources provide superior bioavailability due to absence of phytates that inhibit zinc absorption from plant foods.
Potassium: Electrolyte Balance and Cardiovascular Health
Potassium functions primarily as the principal intracellular cation, maintaining cellular electrochemical gradients essential for nerve transmission, muscle contraction, and acid-base balance. The sodium-potassium ATPase pump actively transports potassium into cells while extruding sodium, consuming approximately 20-40% of resting metabolic energy in adults. This gradient establishes the resting membrane potential in excitable cells (neurons, myocytes) and enables action potential generation.
Epidemiological evidence demonstrates inverse associations between potassium intake and blood pressure, with meta-analyses indicating that increased potassium consumption reduces both systolic and diastolic blood pressure, particularly in hypertensive individuals. The mechanism involves enhanced sodium excretion, direct vasodilation, and reduced sympathetic nervous system activity. Additionally, adequate potassium intake associates with reduced stroke risk, independent of blood pressure effects.
Recommended Intake: The adequate intake level is 2,600 mg daily for women and 3,400 mg for men, though typical Western diets provide only 50-70% of this target, representing a widespread nutritional inadequacy.
Optimal Sources: Potassium distributes widely across minimally processed foods. White potatoes with skin provide 926 mg per medium potato, sweet potatoes offer 542 mg, bananas contain 422 mg per medium fruit, and white beans provide 1,004 mg per cup. Notably, processing typically reduces potassium content substantially, making whole food sources preferable.
Selenium: Antioxidant Defense and Thyroid Metabolism
Selenium incorporates into selenoproteins through the amino acid selenocysteine, often termed the “21st amino acid” due to its unique codon and insertion mechanism. Approximately 25 selenoproteins exist in humans, with glutathione peroxidases representing the most abundant class. These enzymes catalyze the reduction of hydrogen peroxide and organic hydroperoxides, providing critical antioxidant defense against oxidative damage to lipids, proteins, and DNA.
Selenoproteins also include iodothyronine deiodinases, which convert thyroid hormone thyroxine (T4) to its active form triiodothyronine (T3), making selenium essential for thyroid hormone metabolism. Selenium deficiency can impair thyroid function even when iodine status is adequate. Additionally, selenoproteins participate in immune function, reproduction, and possibly cancer prevention, though supplementation trials have yielded mixed results regarding disease prevention.
Recommended Intake: Adults require 55 micrograms daily, a relatively narrow amount above which toxicity risk increases.
Optimal Sources: Brazil nuts provide exceptional selenium concentration—just 1-2 nuts typically supply the recommended daily intake (though content varies substantially based on soil selenium levels where trees grew). Seafood (yellowfin tuna: 92 mcg per 3 ounces), organ meats (beef liver: 28 mcg per 3 ounces), and enriched grains also contribute meaningfully.
Iodine: Thyroid Hormone Synthesis
Iodine’s singular essential function involves thyroid hormone synthesis—it represents the key structural component of thyroxine (T4) and triiodothyronine (T3). The thyroid gland concentrates iodine from circulation through sodium-iodide symporters, achieving concentrations 20-40 times plasma levels. Thyroid hormones regulate metabolic rate, thermogenesis, protein synthesis, and neural development, making adequate iodine essential throughout life, particularly during fetal development and early childhood.
Iodine deficiency represents a persistent global health concern, affecting approximately 2 billion people. Deficiency during pregnancy causes cretinism—severe mental retardation and physical stunting—in offspring, while childhood deficiency impairs cognitive development and growth. In adults, deficiency manifests as hypothyroidism and goiter (thyroid gland enlargement). Universal salt iodization has substantially reduced deficiency prevalence in developed nations, though inadequate intake remains common in regions without iodization programs.
Recommended Intake: Adults require 150 micrograms daily, increasing to 220 mcg during pregnancy and 290 mcg during lactation to support fetal/infant neurodevelopment.
Optimal Sources: Seaweed and seafood provide the richest sources due to iodine concentration in marine environments. One sheet of nori contains 16-43 mcg, while 3 ounces of cod provides approximately 99 mcg. Iodized salt delivers 71 mcg per 1/4 teaspoon. Dairy products contain variable iodine due to iodine supplementation in livestock feed and use of iodine-containing disinfectants in milk production.
Phosphorus: Energy Metabolism and Skeletal Structure
Phosphorus exists in all living cells, primarily as phosphate groups in ATP (the universal energy currency), phospholipids (comprising cell membranes), and nucleic acids (DNA and RNA). Approximately 85% of body phosphorus resides in bone as calcium phosphate (hydroxyapatite), providing skeletal strength while serving as a mineral reservoir. The remaining phosphorus distributes throughout soft tissues, participating in energy transfer reactions, cell signaling pathways, and pH buffering.
Phosphorus absorption efficiency is high (approximately 60-70% across typical dietary intakes), and deficiency is rare in populations consuming adequate protein, as phosphorus distributes widely in protein-containing foods. However, excessive phosphorus intake—particularly as phosphate additives in processed foods—may adversely affect bone health by altering calcium metabolism and associate with cardiovascular disease in individuals with impaired renal function.
Recommended Intake: Adults require 700 mg daily, easily achieved through diverse diets.
Optimal Sources: Protein-rich foods inherently contain substantial phosphorus: chicken breast provides 300 mg per 3 ounces, salmon offers 252 mg, and lentils contain 356 mg per cup. Dairy products (milk: 247 mg per cup) and nuts also contribute significantly. Processed foods containing phosphate additives can provide excessive amounts, warranting mindful consumption.
Copper: Connective Tissue Formation and Iron Metabolism
Copper functions as a cofactor for enzymes catalyzing oxidation-reduction reactions essential for energy production, iron metabolism, neurotransmitter synthesis, and connective tissue formation. Cytochrome c oxidase, the terminal enzyme in the electron transport chain, requires copper for catalytic activity, making copper indispensable for cellular respiration. Ceruloplasmin, a copper-containing ferroxidase, enables iron incorporation into transferrin, linking copper and iron metabolism—copper deficiency can present with anemia resembling iron deficiency.
Additional copper-dependent enzymes include lysyl oxidase (cross-linking collagen and elastin, essential for connective tissue strength), superoxide dismutase (antioxidant defense), dopamine β-hydroxylase (converting dopamine to norepinephrine), and tyrosinase (melanin synthesis). This diversity of functions explains why copper deficiency, though uncommon, produces multisystem manifestations including anemia, neutropenia, skeletal abnormalities, and neurological dysfunction.
Recommended Intake: Adults require 900 micrograms daily.
Optimal Sources: Organ meats represent the richest sources (beef liver: 12,400 mcg per 3 ounces). More commonly consumed sources include oysters (4,850 mcg per 3 ounces), nuts (cashews: 622 mcg per ounce), seeds (sunflower seeds: 519 mcg per ounce), and dark chocolate (501 mcg per ounce).
Manganese: Antioxidant Defense and Metabolism
Manganese serves as a cofactor for enzymes involved in amino acid, cholesterol, and carbohydrate metabolism, as well as antioxidant defense through manganese superoxide dismutase (MnSOD). This mitochondrial enzyme catalyzes superoxide radical conversion to hydrogen peroxide, providing critical protection against oxidative damage in energy-producing organelles. Manganese also activates enzymes involved in bone formation, including glycosyltransferases necessary for proteoglycan synthesis in cartilage and bone matrix.
Additional manganese-dependent enzymes include arginase (urea cycle), pyruvate carboxylase (gluconeogenesis), and various glycosyltransferases (involved in protein glycosylation). Deficiency is extremely rare under normal dietary conditions, though experimentally induced deficiency produces impaired growth, skeletal abnormalities, and altered carbohydrate and lipid metabolism.
Recommended Intake: The adequate intake is 2.3 mg daily for men and 1.8 mg for women.
Optimal Sources: Plant foods generally provide superior manganese content compared to animal products. Whole grains (brown rice: 1.8 mg per cup), nuts (pecans: 1.3 mg per ounce), legumes (chickpeas: 1.7 mg per cup), and certain fruits (pineapple: 0.8 mg per cup) represent excellent sources. Tea also contributes substantially (0.4-1.6 mg per cup depending on variety and brewing time).
Optimizing Mineral Status Through Dietary Strategy
Achieving adequate mineral intake requires attention to both quantity and quality of dietary sources, as well as understanding nutrient interactions.
Whole Food Emphasis and Nutrient Density
Whole, minimally processed foods provide minerals in forms exhibiting superior bioavailability compared to isolated supplements, often accompanied by complementary nutrients enhancing absorption. For instance, meat provides heme iron alongside proteins that enhance absorption, while vegetables supply minerals with vitamin C and other phytochemicals. Building dietary patterns around nutrient-dense whole foods—vegetables, fruits, whole grains, legumes, nuts, seeds, and animal products for those who consume them—generally ensures adequate mineral intake across multiple nutrients simultaneously.
This approach proves more effective than targeting individual minerals through supplementation, which can create imbalances (such as high zinc impairing copper absorption) and lacks the synergistic effects of food matrices. Supplementation remains appropriate for addressing documented deficiencies or meeting elevated requirements during specific life stages (pregnancy, lactation), but should complement rather than replace dietary optimization.
Strategic Combination and Preparation Methods
Enhancing mineral bioavailability through strategic food combinations and preparation methods can substantially improve mineral status. Consuming vitamin C sources with plant-based iron increases absorption several-fold. Soaking, sprouting, or fermenting grains and legumes reduces phytate content, enhancing mineral availability. Conversely, consuming tea or coffee with meals can reduce iron absorption by up to 60% due to polyphenol content—spacing these beverages away from meals preserves mineral absorption.
Additionally, including moderate amounts of protein with mineral-rich plant foods may enhance absorption through amino acid facilitation of mineral transport. These simple modifications to meal composition and timing can yield meaningful improvements in mineral status without requiring major dietary restructuring.
Monitoring and Addressing Mineral Status
While severe mineral deficiencies produce overt clinical manifestations, subclinical insufficiencies can impair health more subtly, warranting awareness of risk factors and assessment approaches.
Populations at Increased Deficiency Risk
Certain demographic groups face elevated risk of mineral inadequacy. Premenopausal women commonly experience iron insufficiency due to menstrual losses. Older adults exhibit increased risk for multiple mineral deficiencies due to reduced food intake, impaired absorption, and medication interactions. Individuals following restrictive diets (vegans, those avoiding entire food groups) require particular attention to minerals predominantly found in excluded foods. People with gastrointestinal disorders affecting absorption (celiac disease, inflammatory bowel disease, gastric bypass) also require monitoring.
Pregnant and lactating women require substantially increased intakes of multiple minerals to support fetal development and milk production. Recognition of these risk factors enables proactive dietary modification or supplementation before deficiency develops.
Laboratory Assessment and Clinical Indicators
When deficiency is suspected, laboratory assessment provides objective status evaluation. Serum ferritin indicates iron stores, though interpretation requires considering inflammatory status (which elevates ferritin independent of iron status). Serum magnesium poorly reflects total body stores (most magnesium is intracellular), making clinical assessment more relevant. Zinc status assessment remains challenging—serum zinc reflects only a small body pool and exhibits diurnal variation.
For most minerals, comprehensive metabolic panels, complete blood counts, and specific mineral assays provide useful information when interpreted by healthcare providers familiar with normal ranges and confounding factors. Self-diagnosis of deficiency based on non-specific symptoms (fatigue, weakness) risks inappropriate supplementation; professional assessment ensures accurate diagnosis and appropriate intervention.
Conclusion
Understanding the physiological roles, recommended intakes, and optimal food sources of essential minerals enables evidence-based dietary choices supporting long-term health. The ten minerals discussed—calcium, iron, magnesium, zinc, potassium, selenium, iodine, phosphorus, copper, and manganese—participate in fundamental biological processes from energy metabolism to immune function, skeletal integrity to antioxidant defense. Achieving adequate status requires consuming nutrient-dense whole foods in sufficient variety, attending to bioavailability factors, and recognizing individual risk factors that may necessitate targeted intervention. By integrating this nutritional knowledge into daily food choices, you can optimize mineral status and support the countless biochemical reactions these inorganic nutrients enable throughout your body.
Important Disclaimer: This article is for informational purposes only and should not replace professional advice. For health-related topics, consult healthcare providers. For financial or legal matters, seek qualified professional guidance. For safety procedures, verify current best practices and local regulations. Individual results may vary, and personal circumstances should always be considered when implementing any suggestions.