Meta Description: Discover how COPD affects more than your lungs, revealing its wide-ranging impact on the heart, muscles, and overall health, with strategies to manage it.
Introduction
Chronic Obstructive Pulmonary Disease (COPD) is often associated with breathing difficulties, chronic cough, and reduced lung capacity. But did you know its effects extend far beyond the lungs? Understanding the systemic impact of COPD is essential for managing overall health and improving quality of life.
COPD doesn’t just make breathing harder; it influences your heart, muscles, metabolism, and even mental well-being. By recognizing the wider impact, you can take proactive steps—like lifestyle adjustments, dietary improvements, and exercise strategies—to mitigate complications and support your body holistically.
This guide explores the far-reaching effects of COPD, explains why early management matters, and offers practical approaches to maintain strength, energy, and overall wellness. Whether you’re newly diagnosed, supporting a loved one, or simply curious about the body’s interconnected systems, this article empowers you to understand and act.
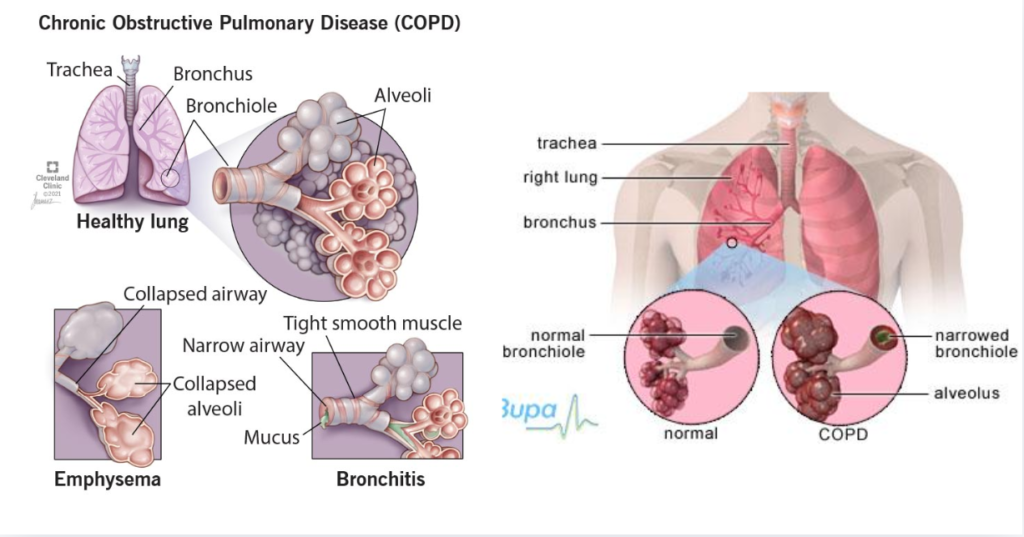
Section 1: Foundation – How COPD Extends Beyond the Lungs
While COPD primarily affects lung tissue, inflammation and reduced oxygen supply ripple through the entire body.
H3: Cardiovascular Strain
Reduced lung function forces the heart to work harder to supply oxygen, often leading to:
- Pulmonary hypertension (high blood pressure in the lungs)
- Increased risk of heart failure
- Elevated resting heart rate and fatigue
H3: Muscle Weakness and Wasting
COPD often contributes to skeletal muscle dysfunction due to:
- Reduced oxygen delivery to muscles
- Inactivity caused by shortness of breath
- Nutritional deficiencies
This can manifest as weakness, fatigue, and reduced mobility, even in muscles unrelated to breathing.
H3: Systemic Inflammation
Chronic lung inflammation triggers widespread effects:
- Joint pain and stiffness
- Increased susceptibility to infections
- Metabolic imbalances that may contribute to diabetes or weight loss
Understanding these foundational impacts helps patients and caregivers anticipate complications and adopt proactive management strategies.
Section 2: Recognizing Key Systemic Symptoms
H3: Cardiovascular Symptoms
- Swelling in the ankles or legs
- Persistent fatigue during light activity
- Chest discomfort or palpitations
H3: Metabolic and Nutritional Changes
- Unintentional weight loss or muscle loss
- Poor appetite due to fatigue or breathlessness
- Vitamin deficiencies that worsen muscle and bone health
H3: Mental Health Implications
- Anxiety related to breathing difficulty
- Depression from reduced physical independence
- Cognitive slowing linked to chronic low oxygen levels
Monitoring these systemic symptoms is crucial because early intervention can significantly improve outcomes.
Section 3: Step-by-Step Management Approaches
H3: Optimizing Lung Health
- Follow prescribed inhaler routines and medications
- Use pulmonary rehabilitation to improve lung efficiency
- Avoid triggers like smoke, dust, and air pollutants
H3: Supporting Cardiovascular Function
- Engage in low-impact exercises like walking, swimming, or cycling
- Monitor blood pressure and heart rate regularly
- Discuss with your doctor about medications that protect heart function
H3: Enhancing Muscle Strength
- Incorporate resistance training or light weight exercises
- Ensure adequate protein intake for muscle maintenance
- Schedule physical therapy if mobility is significantly reduced
H3: Maintaining Mental Well-Being
- Practice stress management techniques: deep breathing, meditation
- Join support groups or counseling sessions
- Engage in hobbies that encourage social interaction and purpose
Section 4: Advanced Strategies and Pro Tips
H3: Nutritional Optimization
- Antioxidant-rich foods (fruits, vegetables) can combat inflammation
- Omega-3 fatty acids may support heart and lung health
- Small, frequent meals help maintain energy and nutrient intake
H3: Personalized Exercise Plans
- Tailor intensity to your current oxygen levels and stamina
- Combine aerobic activity with muscle-strengthening routines
- Use pulse oximetry if needed to monitor oxygen saturation
H3: Integrative Therapies
- Breathing exercises (diaphragmatic or pursed-lip breathing) improve oxygen efficiency
- Yoga or tai chi can support both respiratory and mental health
- Discuss complementary therapies with healthcare providers for safety
Section 5: Troubleshooting Common Challenges
H4: Managing Breathlessness During Activity
- Pace yourself and use rest breaks
- Sit or lean forward to ease lung strain
- Consider supplemental oxygen if prescribed
H4: Coping with Fatigue and Muscle Weakness
- Prioritize daily tasks and conserve energy
- Implement gentle stretching routines
- Seek guidance from a physiotherapist for progressive strengthening
H4: Preventing Exacerbations
- Get annual flu and pneumonia vaccinations
- Avoid infections through hygiene and avoiding crowded spaces
- Track symptoms for early signs of flare-ups
Section 6: Maximizing Long-Term Outcomes
H3: Lifestyle Adjustments
- Maintain a smoke-free environment
- Optimize sleep to support recovery and energy
- Hydrate consistently to support mucous clearance
H3: Routine Medical Monitoring
- Regular check-ups for lung function, heart health, and nutrition
- Screening for osteoporosis, diabetes, and other systemic complications
- Adjust treatments as symptoms evolve
H3: Empowering Yourself Through Education
- Learn about COPD triggers and early warning signs
- Understand the interaction between systemic health and lung function
- Advocate for personalized care and rehabilitation programs
Internal Linking Opportunities
- “Pulmonary Rehabilitation: Reclaiming Breath and Strength”
- “Nutrition Tips for Chronic Illness Management”
- “Mental Health Strategies for Chronic Respiratory Conditions”
- “Exercise Adaptations for Limited Mobility”
- “Preventing Infections in Vulnerable Populations”
Featured Snippet: How Does COPD Affect the Whole Body?
COPD impacts more than the lungs—it places strain on the heart, leads to muscle weakness, causes systemic inflammation, affects metabolism, and can contribute to mental health challenges. Understanding these systemic effects allows for early interventions that improve quality of life and overall health.
Conclusion
COPD is a complex condition that reaches far beyond lung function. By recognizing its systemic effects—on the heart, muscles, metabolism, and mental well-being—you can adopt a holistic approach to health. Incorporating proper medical management, tailored exercise, nutritional support, and mental wellness strategies empowers you to maintain independence, improve energy, and enhance overall quality of life.
Understanding your body’s interconnected systems and acting proactively ensures that you’re not just managing COPD—you’re thriving despite it. Take charge today, and embrace strategies that support every part of your body for long-term wellness.
Important Disclaimer: This article is for informational purposes only and should not replace professional advice. For health-related topics, consult healthcare providers. Individual results may vary, and personal circumstances should always be considered when implementing any suggestions.