A well-structured celiac disease diet eliminates gluten while preserving nutrition, protecting intestinal health, and supporting long-term wellness.
For individuals diagnosed with celiac disease, food is more than nourishment—it is medicine. Celiac disease is an autoimmune condition triggered by gluten, a protein found in wheat, barley, and rye. Even trace amounts can provoke immune-mediated damage to the small intestine, leading to malabsorption, systemic inflammation, and long-term complications. Successfully navigating the celiac disease diet requires scientific understanding, practical planning, and informed food choices. This comprehensive guide explores safe foods, risk factors, nutritional considerations, and evidence-based strategies for living well without gluten.
Section 1: What Is Celiac Disease and How Does Gluten Cause Harm?
Celiac disease is a chronic autoimmune disorder in which ingestion of gluten triggers an immune attack on the small intestine’s lining.
H3: The Autoimmune Mechanism
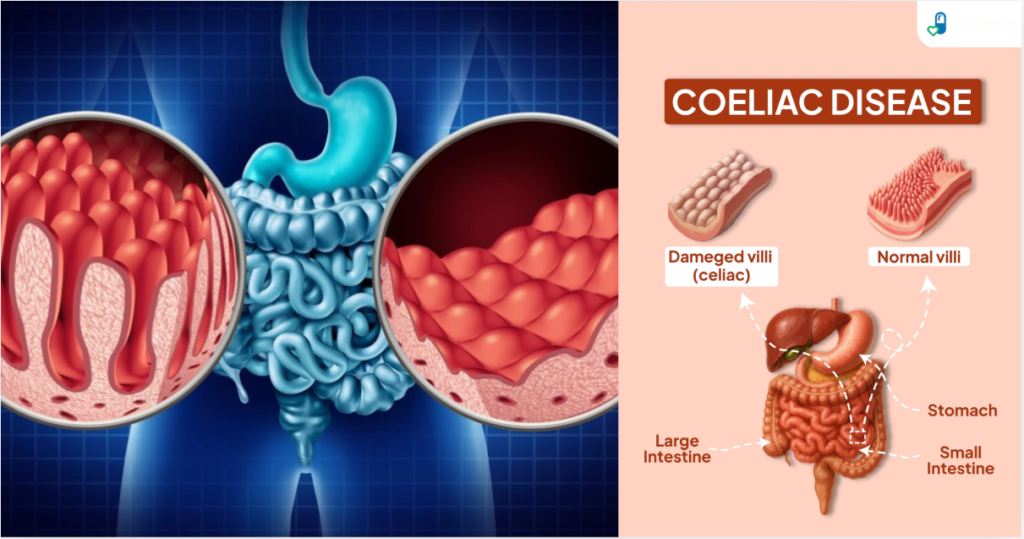
When gluten is consumed, the immune system mistakenly identifies fragments of the protein as harmful. This reaction damages the villi—small, finger-like projections lining the small intestine that are responsible for nutrient absorption.
H3: Consequences of Intestinal Damage
Damaged villi impair absorption of essential nutrients such as iron, calcium, folate, and fat-soluble vitamins. Over time, untreated celiac disease can lead to anemia, osteoporosis, infertility, neurological symptoms, and increased risk of certain cancers.
Strict adherence to a gluten-free diet is currently the only effective treatment.
Section 2: What Foods Must Be Avoided on a Celiac Disease Diet?
The cornerstone of managing celiac disease is complete elimination of gluten-containing grains.
Primary Sources of Gluten:
- Wheat (including spelt, farro, semolina, durum)
- Barley
- Rye
- Triticale
Hidden Sources of Gluten:
- Processed sauces and gravies
- Soy sauce
- Malt products
- Certain medications and supplements
- Processed meats and flavorings
Even minimal exposure can trigger intestinal inflammation. Careful label reading and awareness of cross-contamination risks are essential.
Section 3: What Are Safe Foods for People with Celiac Disease?
A well-balanced celiac disease diet includes a wide variety of naturally gluten-free foods.
H3: Naturally Gluten-Free Whole Foods
- Fresh fruits and vegetables
- Unprocessed meat, poultry, and fish
- Eggs
- Dairy (if tolerated)
- Legumes
- Nuts and seeds
H3: Gluten-Free Grains and Starches
- Rice
- Quinoa
- Buckwheat
- Millet
- Amaranth
- Corn
- Certified gluten-free oats
These foods form the nutritional backbone of a healthy gluten-free lifestyle, ensuring adequate fiber, protein, and micronutrient intake.
Section 4: How Does Cross-Contamination Occur and How Can It Be Prevented?
Cross-contamination happens when gluten-free foods come into contact with gluten-containing products.
Common Sources of Cross-Contact:
- Shared toasters
- Cutting boards
- Frying oil used for breaded foods
- Bulk food bins
- Restaurant kitchens
Prevention Strategies:
- Use dedicated cookware and utensils
- Store gluten-free foods separately
- Communicate dietary needs clearly when dining out
- Choose certified gluten-free products
Vigilance in both home and public settings significantly reduces accidental exposure.
Section 5: Which Nutritional Deficiencies Are Common in Celiac Disease?
Due to prior intestinal damage and dietary restrictions, individuals with celiac disease may face nutritional gaps.
Common Deficiencies:
- Iron (leading to anemia)
- Calcium and Vitamin D (affecting bone health)
- Vitamin B12 and folate
- Zinc and magnesium
A nutrient-dense, balanced gluten-free diet, sometimes supplemented under medical supervision, helps restore optimal nutritional status.
Section 6: How Does the Gut Heal on a Gluten-Free Diet?
Once gluten is eliminated, the intestinal lining begins to recover.
H3: Timeline of Healing
Children often experience faster recovery, while adults may require months to years for complete mucosal healing.
H3: Symptom Improvement
Digestive symptoms such as bloating, diarrhea, and abdominal pain typically improve within weeks. However, silent intestinal damage may persist if gluten exposure continues unintentionally.
Adherence consistency is critical for long-term remission and prevention of complications.
Section 7: What Smart Choices Support Long-Term Success?
Sustainable management of celiac disease extends beyond avoiding gluten.
H3: Emphasize Whole Foods Over Processed Alternatives
Many packaged gluten-free products are high in sugar and refined starch. Prioritizing whole foods ensures better glycemic control and nutrient density.
H3: Plan Balanced Meals
Include:
- Lean proteins
- Fiber-rich vegetables
- Healthy fats
- Gluten-free whole grains
H3: Build a Support Network
Registered dietitians, support groups, and educational resources provide practical guidance and emotional support.
Adopting a proactive and informed approach transforms dietary restriction into a structured wellness strategy.
Section 8: Which Lifestyle and Medical Considerations Are Important?
Living with celiac disease involves ongoing monitoring and healthcare collaboration.
Medical Follow-Up:
- Regular antibody testing to confirm dietary adherence
- Bone density screenings
- Nutrient level monitoring
Lifestyle Awareness:
- Educating family and friends
- Advocating for safe options in social settings
- Managing stress, which may exacerbate symptoms
A coordinated approach between patient and healthcare provider ensures comprehensive management.
Conclusion: Building Confidence and Health on a Celiac Disease Diet
Navigating the celiac disease diet requires diligence, education, and thoughtful food selection. By eliminating gluten, preventing cross-contamination, and prioritizing nutrient-dense whole foods, individuals with celiac disease can restore intestinal health and prevent long-term complications. With proper planning and medical support, a gluten-free lifestyle becomes not a limitation but a structured pathway toward improved vitality and well-being.
Important Disclaimer
This article is for informational purposes only and does not replace professional medical advice. Individuals with suspected or diagnosed celiac disease should consult a qualified healthcare provider or registered dietitian for personalized evaluation and treatment guidance.