Ovarian cancer often develops silently, but recognizing early signs and understanding risk factors can dramatically improve outcomes and empower prevention.
Ovarian cancer is sometimes called the “silent disease” because its symptoms can be subtle and easy to overlook. Many women dismiss early changes as digestive discomfort, hormonal shifts, or normal aging. But when it comes to ovarian cancer, awareness is power.
Understanding the early signs, knowing your personal risk factors, and taking proactive steps toward prevention can make a life-saving difference. While there is no guaranteed way to prevent ovarian cancer, early detection and healthy lifestyle choices can significantly improve outcomes. This guide will walk you through everything you need to know—clearly, confidently, and with actionable steps you can take today.
What Is Ovarian Cancer and Why Is It Often Missed?
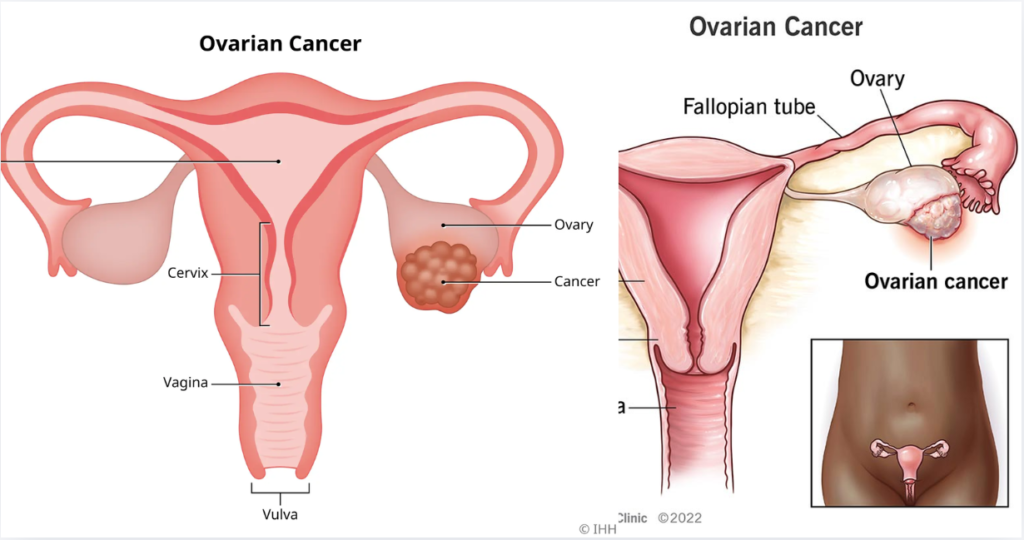
Ovarian cancer begins in the ovaries or nearby tissues such as the fallopian tubes. It occurs when abnormal cells grow uncontrollably and form a tumor. There are different types, but epithelial ovarian cancer is the most common.
Why Is Ovarian Cancer Hard to Detect Early?
Unlike cervical cancer, there is no routine, highly effective screening test for ovarian cancer in the general population. Symptoms are often vague and may include bloating or mild abdominal discomfort—things many people experience occasionally.
Because of this, ovarian cancer is frequently diagnosed at a later stage, when treatment becomes more complex.
Who Is Most Commonly Affected?
Ovarian cancer primarily affects women over age 50, especially after menopause. However, it can occur at younger ages, particularly in those with genetic risk factors.
Understanding your body and noticing persistent changes is crucial.
What Are the Early Signs of Ovarian Cancer?
Recognizing early symptoms can improve early detection.
Quick Answer (Featured Snippet Potential)
Early signs of ovarian cancer may include persistent bloating, pelvic or abdominal pain, feeling full quickly when eating, frequent urination, unexplained fatigue, and changes in bowel habits. Symptoms that last more than two weeks should be evaluated by a healthcare provider.
Most Common Early Symptoms
Be aware of these persistent changes:
- Ongoing abdominal bloating
- Pelvic or lower abdominal pain
- Difficulty eating or feeling full quickly
- Increased urinary urgency or frequency
- Unexplained weight loss or gain
- Fatigue
Occasional bloating is normal. Persistent bloating that does not resolve is not.
Less Common but Important Symptoms
- Back pain
- Menstrual changes (if premenopausal)
- Pain during intercourse
- Changes in bowel habits
If symptoms occur almost daily for two weeks or more, it’s important to seek medical advice.
What Are the Main Risk Factors for Ovarian Cancer?
Understanding risk factors helps you assess your personal risk and discuss preventive strategies with your doctor.
Age and Menopause
Risk increases with age. Most ovarian cancer cases occur after menopause.
Family History and Genetics
Women with a family history of ovarian, breast, or colorectal cancer have a higher risk.
BRCA1 and BRCA2 gene mutations significantly increase ovarian cancer risk. Genetic testing may be recommended if you have a strong family history.
This topic connects closely to related articles on genetic cancer risk and BRCA mutation testing.
Reproductive History
Certain reproductive factors may influence risk:
- Never having been pregnant
- Early menstruation
- Late menopause
- Endometriosis
Conversely, pregnancy and breastfeeding may lower risk.
Hormone Therapy
Long-term use of estrogen-only hormone replacement therapy (HRT) after menopause may increase ovarian cancer risk.
Discuss risks and benefits carefully with your healthcare provider.
How Is Ovarian Cancer Diagnosed?
Early diagnosis can improve survival rates.
Step 1: Medical Evaluation
If symptoms persist, your doctor may:
- Conduct a pelvic exam
- Order a transvaginal ultrasound
- Request blood tests such as CA-125
CA-125 is not a perfect screening test but may help in evaluation.
Step 2: Imaging Tests
Ultrasound or CT scans help identify ovarian masses. Not all masses are cancerous—many are benign cysts.
Step 3: Surgical Confirmation
Definitive diagnosis usually requires surgery and biopsy. If cancer is confirmed, staging determines how far it has spread.
Early-stage ovarian cancer has a significantly better prognosis than advanced-stage disease.
Can Ovarian Cancer Be Prevented?
There is no guaranteed way to prevent ovarian cancer, but certain strategies may reduce risk.
Oral Contraceptives
Long-term use of birth control pills has been shown to reduce ovarian cancer risk. However, they carry other risks and benefits that should be discussed individually.
Risk-Reducing Surgery
Women with BRCA mutations may consider preventive removal of ovaries and fallopian tubes after completing childbearing. This significantly lowers risk.
Healthy Lifestyle Habits
While lifestyle changes cannot eliminate genetic risk, they support overall cancer prevention:
- Maintain a healthy weight
- Exercise regularly
- Eat a diet rich in fruits and vegetables
- Avoid smoking
These habits also reduce the risk of other cancers and chronic diseases.
For broader prevention strategies, this topic aligns well with articles on anti-inflammatory diets, cancer prevention lifestyle tips, and women’s preventive health screenings.
Common Challenges and Misconceptions
“I Don’t Have a Family History, So I’m Not at Risk.”
Most women diagnosed with ovarian cancer do not have a known genetic mutation. Awareness still matters.
“Bloating Is Normal, So I Shouldn’t Worry.”
Occasional bloating is common. Persistent, unusual bloating that differs from your normal pattern deserves attention.
“There’s No Screening Test, So There’s Nothing I Can Do.”
While routine screening isn’t available for everyone, knowing your body and reporting persistent symptoms early is powerful.
Maximizing Early Detection and Prevention
You can take proactive steps today.
Track Symptoms
If you notice changes, write them down. Track:
- Frequency
- Duration
- Severity
Patterns help doctors make informed decisions.
Stay Up to Date on Check-Ups
Annual gynecologic exams are important, even after menopause.
Know Your Family History
Discuss any family history of breast, ovarian, or colorectal cancer with relatives. Share this information with your healthcare provider.
Consider Genetic Counseling
If you have multiple relatives with related cancers, genetic counseling may clarify your risk.
Knowledge reduces uncertainty and guides prevention.
Emotional Well-Being and Ovarian Cancer Awareness
Fear around cancer is understandable. But awareness is not about panic—it’s about preparation and empowerment.
Taking action early does not mean expecting the worst. It means valuing your health.
When you stay informed, track symptoms, and seek medical advice promptly, you significantly improve your chances of early detection and successful treatment if needed.
Conclusion: Awareness Is Your Strongest Defense
Ovarian cancer may be subtle in its early stages, but it is not invisible. By understanding early signs, recognizing risk factors, and embracing preventive strategies, you give yourself a powerful advantage.
Listen to your body. Notice persistent changes. Stay proactive with regular medical care. While not all cases can be prevented, early action can dramatically improve outcomes.
You have the ability to protect your health through awareness, education, and timely care. That knowledge is empowering—and potentially life-saving.
Important Disclaimer: This article is for informational purposes only and should not replace professional advice. For health-related topics, consult healthcare providers. For financial or legal matters, seek qualified professional guidance. For safety procedures, verify current best practices and local regulations. Individual results may vary, and personal circumstances should always be considered when implementing any suggestions.