Meta Description: Discover celiac disease symptoms, causes, and how to manage a gluten-free life. Learn practical tips to improve digestion, health, and daily living.
Introduction
Living with digestive discomfort, fatigue, or unexplained health issues can feel overwhelming. For many people, the hidden cause may be Celiac Disease, a serious autoimmune condition triggered by gluten.
This article will guide you through the symptoms, causes, and management of celiac disease, helping you understand how your body reacts and what steps you can take to feel better. With the right knowledge and lifestyle changes, you can regain control of your health and enjoy a full, balanced life—even on a gluten-free diet.
Section 1: Understanding Celiac Disease
H3: What Is Celiac Disease?
Celiac disease is an autoimmune disorder where the immune system attacks the small intestine when gluten is consumed. Gluten is a protein found in wheat, barley, and rye.
Over time, this reaction damages the intestinal lining, making it harder for your body to absorb nutrients properly.
H3: Why It Matters
- Leads to nutrient deficiencies (iron, calcium, vitamins)
- Can affect multiple body systems beyond digestion
- Requires lifelong dietary management
H3: Who Is at Risk?
- People with a family history of celiac disease
- Individuals with autoimmune conditions
- Those with genetic predisposition
Section 2: Symptoms You Should Never Ignore
H3: Digestive Symptoms
- Chronic diarrhea or constipation
- Bloating and abdominal pain
- Nausea and vomiting
H3: Non-Digestive Symptoms
- Fatigue and weakness
- Anemia (iron deficiency)
- Skin rash (dermatitis herpetiformis)
- Joint pain and headaches
H3: Silent or Atypical Cases
Some people have no obvious digestive symptoms but still suffer internal damage. This makes early diagnosis challenging and highlights the importance of awareness.
Section 3: Causes and Triggers
H3: The Role of Gluten
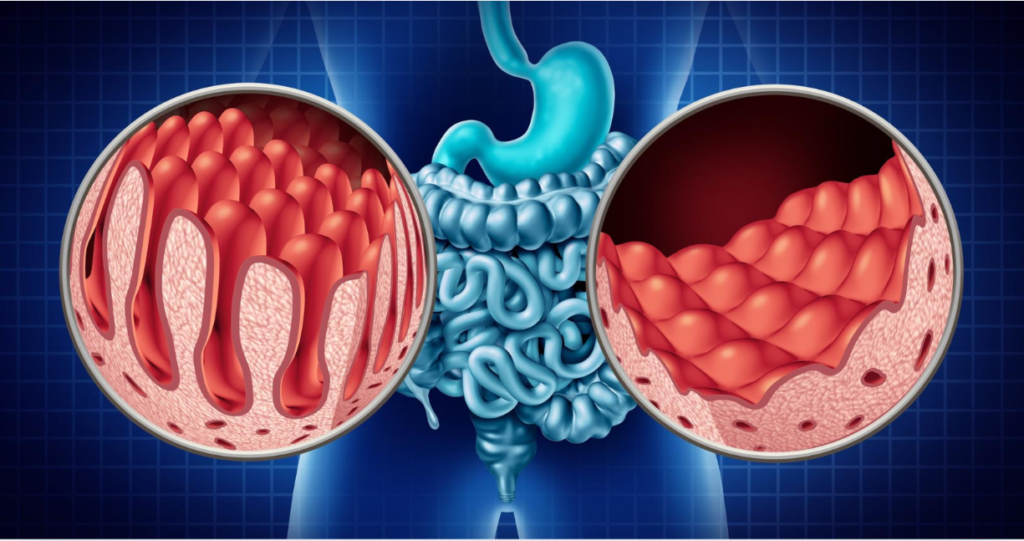
Gluten triggers an immune response that damages the villi (tiny structures in the small intestine responsible for nutrient absorption).
H3: Genetic Factors
- Presence of specific genes (HLA-DQ2 or HLA-DQ8) increases risk
- However, not everyone with these genes develops the disease
H3: Environmental Triggers
- Infections or stress may activate the condition
- Early dietary exposure patterns may play a role
Section 4: Diagnosis and Common Challenges
H3: How Is Celiac Disease Diagnosed?
- Blood tests for specific antibodies
- Intestinal biopsy to confirm damage
- Genetic testing in some cases
Important: You must be eating gluten before testing to ensure accurate results.
H3: Common Challenges
- Misdiagnosis as irritable bowel syndrome (IBS)
- Delayed diagnosis due to mild or unusual symptoms
- Difficulty maintaining a strict gluten-free diet
H3: Emotional Impact
Adjusting to a lifelong condition can feel stressful. But with the right mindset and support, it becomes manageable and empowering.
Section 5: Managing a Gluten-Free Life
H3: What Foods to Avoid
- Wheat (bread, pasta, pastries)
- Barley (soups, malt products)
- Rye (certain breads and cereals)
H3: Safe and Healthy Alternatives
- Rice, quinoa, corn, and gluten-free oats
- Fresh fruits and vegetables
- Lean proteins like fish, eggs, and legumes
H3: Practical Daily Tips
- Always read food labels carefully
- Avoid cross-contamination in the kitchen
- Choose certified gluten-free products
Section 6: Advanced Strategies for Better Living
H3: Nutritional Optimization
- Focus on iron, calcium, vitamin D, and B vitamins
- Consider supplements if recommended by a doctor
H3: Dining Out Safely
- Inform restaurant staff about your condition
- Ask about food preparation methods
- Choose simple, naturally gluten-free dishes
H3: Long-Term Wellness
- Maintain regular medical follow-ups
- Monitor symptoms and nutrient levels
- Build a supportive environment with family and friends
Featured Snippet: What Is the Best Treatment for Celiac Disease?
The only effective treatment for celiac disease is a strict, lifelong gluten-free diet. Avoiding gluten completely allows the intestine to heal, reduces symptoms, and prevents complications.
Section 7: Troubleshooting Common Setbacks
- Accidental gluten exposure: May cause symptoms—return to a strict diet immediately
- Persistent symptoms: Check for hidden gluten or consult a healthcare provider
- Nutrient deficiencies: Address with diet or supplements
Encouragement Tip: Progress takes time. Your body needs patience to heal, and every small step counts.
Section 8: Maximizing Your Health Journey
- Combine a gluten-free diet with a balanced, whole-food lifestyle
- Stay active to support digestion and energy
- Practice stress management for overall well-being
Internal Linking Opportunities:
Explore related topics like gut health improvement, anti-inflammatory diets, managing food intolerances, digestive wellness tips, and immune system support.
Conclusion
Living with celiac disease may feel challenging at first, but it also opens the door to a healthier, more mindful lifestyle. By understanding your body, avoiding gluten, and making smart dietary choices, you can protect your health and thrive.
Takeaway: You have the power to manage celiac disease effectively. With awareness, consistency, and the right habits, you can enjoy a vibrant, balanced, and fulfilling life—completely gluten-free.
Important Disclaimer: This article is for informational purposes only and should not replace professional medical advice. Consult a healthcare provider for diagnosis, treatment, or dietary guidance related to celiac disease.