Meta Description: Learn the symptoms of Polycystic Ovary Syndrome (PCOS), clinical presentation, key indicators, hormonal signs, and how this condition affects women’s health.
Polycystic Ovary Syndrome (PCOS) is one of the most common hormonal disorders affecting women of reproductive age. Yet, it often goes undiagnosed for years because its symptoms can vary widely from one person to another.
Understanding the symptoms of Polycystic Ovary Syndrome is essential for early recognition and proper management. PCOS is not just a reproductive condition—it affects metabolism, hormones, skin, and even emotional well-being.
In this article, you’ll discover the key clinical signs of PCOS, how it presents in the body, and what indicators doctors look for during diagnosis.
What Is Polycystic Ovary Syndrome (PCOS)?
PCOS is a hormonal imbalance condition where the ovaries produce higher-than-normal levels of androgens (male hormones), which can interfere with normal ovulation.
What happens in PCOS?
In many cases:
- Ovulation becomes irregular or stops
- Small fluid-filled sacs (follicles) may develop on ovaries
- Hormonal imbalance affects multiple body systems
Why PCOS matters
PCOS can influence:
- Menstrual cycles
- Fertility
- Skin health
- Weight regulation
- Metabolic function
Featured Snippet: What are the main symptoms of PCOS?
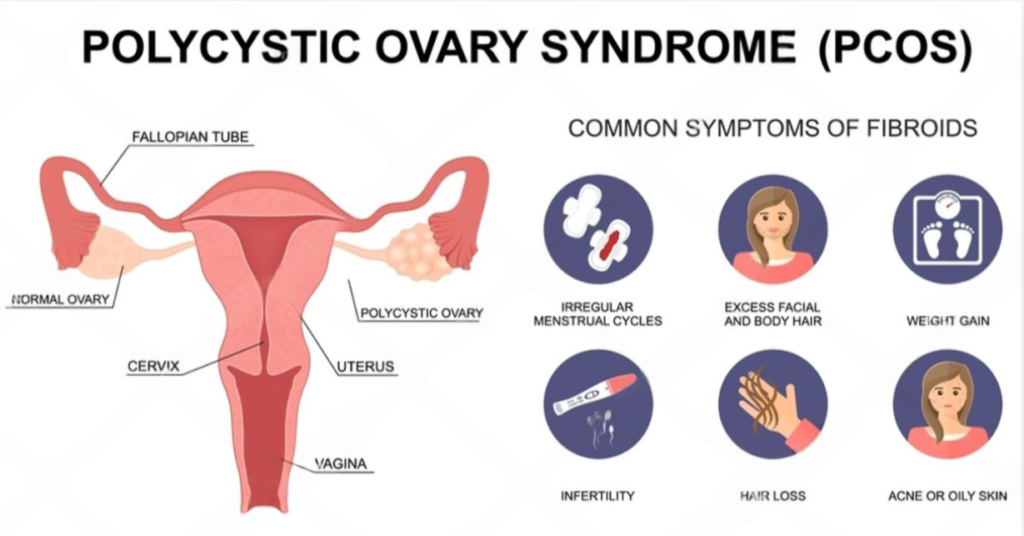
The main symptoms of Polycystic Ovary Syndrome include irregular periods, excess hair growth (hirsutism), acne, weight gain, ovarian cysts, and difficulty with ovulation or fertility.
Clinical Presentation of PCOS
The clinical presentation of PCOS varies, but doctors typically identify a combination of reproductive, hormonal, and metabolic symptoms.
1. Menstrual irregularities
One of the earliest and most common signs is irregular menstruation.
Common cycle patterns include:
- Missed periods (amenorrhea)
- Infrequent periods (oligomenorrhea)
- Heavy or unpredictable bleeding
Why this happens
Hormonal imbalance prevents regular ovulation, which disrupts the menstrual cycle.
2. Signs of elevated androgens (male hormones)
PCOS often leads to higher androgen levels.
Physical signs include:
- Excess facial or body hair (hirsutism)
- Acne, especially on face, chest, or back
- Oily skin
- Hair thinning on the scalp
Why androgens matter
These hormones influence hair growth patterns and skin oil production.
3. Ovarian changes
Not all women with PCOS have cysts, but many show ovarian changes.
What doctors may see on ultrasound:
- Enlarged ovaries
- Multiple small follicles (“string of pearls” appearance)
- Irregular ovulation patterns
Important note
The presence of cysts alone is not enough for diagnosis.
4. Weight and metabolic symptoms
Many women with PCOS experience metabolic changes.
Common symptoms:
- Weight gain or difficulty losing weight
- Increased abdominal fat
- Insulin resistance
- Fatigue after meals
Why metabolism is affected
PCOS is often linked to insulin resistance, which affects how the body processes sugar.
5. Fertility and ovulation issues
PCOS is a leading cause of infertility due to irregular ovulation.
Possible reproductive challenges:
- Difficulty conceiving
- Unpredictable ovulation
- Reduced egg release (anovulation)
6. Skin and cosmetic changes
Hormonal imbalance often affects skin appearance.
Common signs:
- Persistent acne
- Darkened skin patches (acanthosis nigricans)
- Skin tags in folds of skin
Step-by-Step: How PCOS Is Diagnosed
Doctors use a combination of clinical, hormonal, and imaging tests.
Step 1: Clinical evaluation
Doctors assess:
- Menstrual history
- Physical signs (hair growth, acne, weight changes)
- Family history
Step 2: Hormonal blood tests
Key hormones evaluated:
- Androgens (testosterone)
- LH and FSH levels
- Insulin levels (in some cases)
- Thyroid and prolactin (to rule out other conditions)
Step 3: Pelvic ultrasound
Used to check:
- Ovarian structure
- Follicle count
- Uterine health
Advanced Insights: PCOS and Whole-Body Health
PCOS is not just a reproductive issue—it affects multiple systems.
1. Emotional and mental health impact
Women with PCOS may experience:
- Anxiety
- Depression
- Low self-esteem due to physical symptoms
2. Cardiometabolic risk
PCOS is associated with increased risk of:
- Type 2 diabetes
- High cholesterol
- Blood pressure issues
3. Inflammation connection
Research suggests low-grade inflammation may play a role in PCOS progression.
Common Misconceptions About PCOS
Many misunderstand this condition.
Myth 1: PCOS always means ovarian cysts
Not always—some women with PCOS have no visible cysts.
Myth 2: PCOS only affects fertility
It also impacts metabolism, skin, and mental health.
Myth 3: Weight gain is inevitable
While common, lifestyle and medical support can help manage weight.
Internal Linking Opportunities
This topic connects well with:
- Hormonal imbalance and endocrine health
- Insulin resistance and metabolic syndrome
- Female reproductive health and fertility
- Skin health and hormonal acne
- Nutrition for hormonal balance
Conclusion
Understanding the symptoms of Polycystic Ovary Syndrome helps identify the condition early and manage it effectively. From irregular menstrual cycles and hormonal acne to metabolic changes and fertility challenges, PCOS presents in many different ways.
Because it affects multiple systems in the body, early awareness and proper medical evaluation are essential for long-term health and well-being.
With the right combination of lifestyle changes, medical guidance, and consistent care, women with PCOS can successfully manage symptoms and support hormonal balance, energy, and overall quality of life.