Meta Description: Learn about bacterial inflammation, its symptoms, causes, treatment options, and patient care guidelines to support recovery and prevent complications.
Bacterial inflammation is the body’s natural immune response to bacterial invasion. While inflammation is essential for fighting infections, excessive or uncontrolled inflammation can lead to tissue damage and serious complications if not properly managed.
Understanding bacterial inflammation, its symptoms, and appropriate treatment strategies is crucial for early intervention and effective patient care. From localized infections like skin abscesses to systemic conditions, recognizing warning signs can make a significant difference in outcomes.
In this article, we’ll explore the mechanisms behind bacterial inflammation, common symptoms, treatment approaches, and practical patient care guidelines.
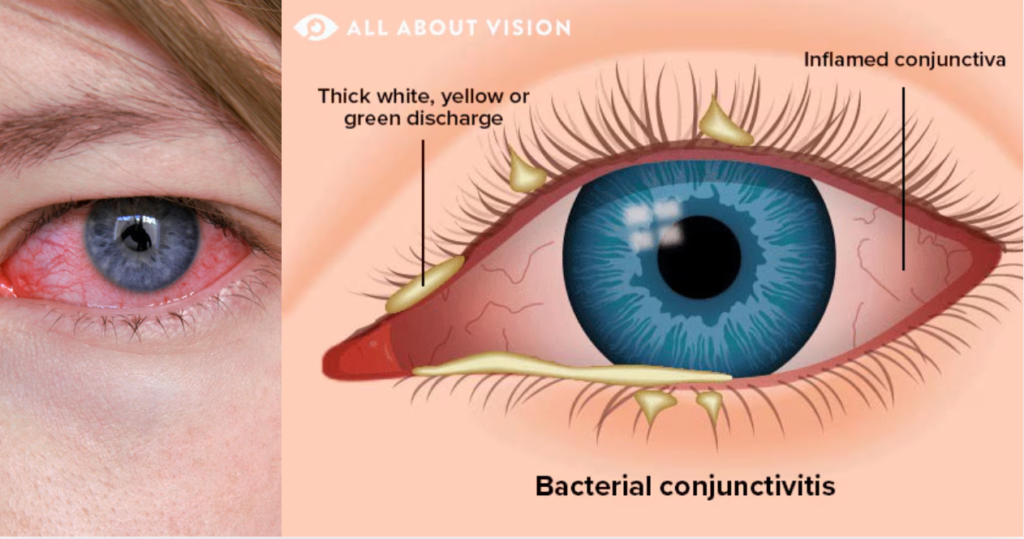
What Is Bacterial Inflammation?
Bacterial inflammation occurs when the immune system responds to harmful bacteria entering the body.
Key processes involved
- Activation of immune cells (neutrophils, macrophages)
- Release of inflammatory mediators (cytokines)
- Increased blood flow to affected tissues
Purpose of inflammation
- Eliminate pathogens
- Remove damaged tissue
- Initiate healing process
Featured Snippet: What are the symptoms of bacterial inflammation?
Symptoms of bacterial inflammation include redness, swelling, pain, warmth, fever, fatigue, and sometimes pus formation, depending on the site and severity of infection.
Common Symptoms of Bacterial Inflammation
Symptoms may vary depending on the infection site but often include classic inflammatory signs.
1. Local symptoms
At the infection site
- Redness (erythema)
- Swelling (edema)
- Warmth
- Pain or tenderness
2. Systemic symptoms
When inflammation spreads:
- Fever
- Chills
- Fatigue
- Loss of appetite
3. Advanced or severe signs
- Pus formation
- Tissue damage
- Rapid heart rate
- Confusion (in severe systemic infection)
Causes and Risk Factors
1. Bacterial infections
Common bacteria include:
- Staphylococcus aureus
- Escherichia coli
- Streptococcus species
2. Entry points for bacteria
- Cuts or wounds
- Respiratory tract
- Digestive tract
- Urinary tract
3. Risk factors
- Weakened immune system
- Chronic diseases
- Poor hygiene
- Hospital exposure
How Bacterial Inflammation Develops
Step 1: Bacterial invasion
Bacteria enter the body through a breach or natural opening.
Step 2: Immune activation
The immune system detects bacteria and releases inflammatory mediators.
Step 3: Local response
- Blood vessels dilate
- Immune cells accumulate
- Tissue becomes inflamed
Step 4: Resolution or progression
- Infection is controlled and healing begins
- Or inflammation spreads if untreated
Treatment of Bacterial Inflammation
Treatment depends on the severity and location of infection.
1. Antibiotic therapy
Antibiotics target and eliminate bacteria.
Important considerations
- Must be prescribed by a healthcare professional
- Full course should be completed
- Misuse can lead to resistance
2. Anti-inflammatory support
- Pain relievers (as prescribed)
- Rest and hydration
3. Drainage procedures
For abscesses:
- Surgical drainage may be required
- Helps remove pus and reduce pressure
4. Hospital care (severe cases)
In serious infections:
- Intravenous antibiotics
- Monitoring vital signs
- Supportive care
Featured Snippet: How is bacterial inflammation treated?
Bacterial inflammation is treated primarily with antibiotics, along with supportive care such as rest, hydration, and in some cases surgical drainage or hospitalization for severe infections.
Patient Care Guidelines
1. Early recognition
Patients should monitor for:
- Increasing pain or swelling
- Fever
- Worsening symptoms
2. Medication adherence
- Take antibiotics exactly as prescribed
- Avoid skipping doses
3. Hygiene practices
- Clean wounds properly
- Wash hands regularly
- Avoid spreading infection
4. Rest and recovery
- Allow the body time to heal
- Maintain proper nutrition
5. Follow-up care
- Attend medical check-ups
- Monitor for recurrence
Advanced Insights into Inflammatory Response
1. Role of cytokines
Cytokines regulate inflammation and immune communication.
2. Acute vs chronic inflammation
- Acute: short-term, protective
- Chronic: prolonged, potentially damaging
3. Systemic inflammatory response
Severe infections may lead to widespread inflammation affecting multiple organs.
Common Complications
1. Abscess formation
Localized pus collection requiring drainage.
2. Sepsis
A life-threatening condition caused by systemic infection.
3. Tissue damage
Prolonged inflammation may harm surrounding tissues.
Internal Linking Opportunities
This topic connects well with:
- Immune system and inflammation mechanisms
- Antibiotic resistance and proper use
- Wound care and infection prevention
- Sepsis and systemic infections
- Chronic inflammation and disease
Conclusion
Bacterial inflammation is a vital defense mechanism, but when uncontrolled, it can lead to serious health complications. Recognizing early symptoms such as redness, swelling, pain, and fever is essential for timely treatment.
With appropriate medical care—including antibiotics, proper hygiene, and supportive recovery strategies—most bacterial inflammatory conditions can be effectively managed. Patient awareness and adherence to treatment play a crucial role in preventing complications and ensuring full recovery.
Understanding how the body responds to infection empowers individuals to act quickly and protect their overall health.
Important Disclaimer: This article is for informational purposes only and should not replace professional medical advice. For diagnosis and treatment of bacterial infections, consult a qualified healthcare provider.