Meta Description: Arnold’s Syndrome, also known as Occipital Neuralgia, is a painful condition that affects the nerves at the base of your skull. Learn about its causes, symptoms, and treatment options for relief.
Arnold’s Syndrome, more commonly known as occipital neuralgia, is a condition that causes intense pain in the back of the head, neck, and sometimes the face. It occurs when the occipital nerves—located at the base of your skull—become irritated or damaged. This condition can cause debilitating symptoms, often mistaken for tension headaches or migraines. Understanding the causes, symptoms, and treatment options is vital for anyone experiencing this type of pain.
In this article, we’ll explore the underlying causes of Arnold’s Syndrome, how to recognize the symptoms, and the most effective treatment options to alleviate the pain and manage the condition. Let’s dive in and understand more about this challenging condition.
What Is Arnold’s Syndrome (Occipital Neuralgia)?
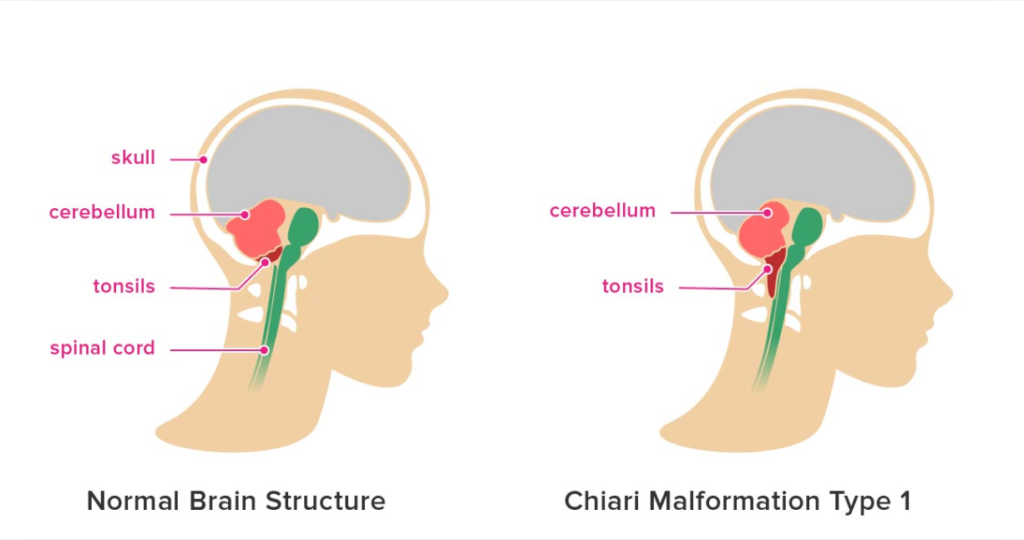
Occipital neuralgia, also referred to as Arnold’s Syndrome, is characterized by irritation or damage to the occipital nerves. These nerves run from the spinal cord to the scalp, passing through the upper neck. When irritated, they can cause severe, sharp, stabbing pain at the back of the head, neck, and sometimes behind the eyes.
Key Features of Occipital Neuralgia:
- Pain at the base of the skull
- Sharp, stabbing headaches
- Pain may radiate to the scalp, forehead, or behind the eyes
The pain from Arnold’s Syndrome is often described as “electric shock-like,” and can last from a few seconds to several minutes. In some cases, the pain can persist for hours or even days.
Causes of Arnold’s Syndrome (Occipital Neuralgia)
The condition occurs when the occipital nerves become inflamed, compressed, or irritated. Understanding the causes is crucial for identifying the underlying issue and treating the condition effectively.
Common Causes Include:
- Trauma or Injury: A whiplash injury, head trauma, or any neck injury that causes compression of the occipital nerves can lead to occipital neuralgia.
- Muscle Tightness: Chronic tension in the neck muscles, such as from poor posture or prolonged neck strain, can irritate the occipital nerves.
- Nerve Compression: Conditions like herniated discs, arthritis, or bone spurs in the cervical spine may lead to compression of the occipital nerves.
- Infection or Inflammation: Viral infections, such as shingles, can affect the occipital nerves, leading to inflammation and pain.
- Diabetes and Other Conditions: Certain health conditions that affect nerve function, such as diabetes or multiple sclerosis, can increase the risk of occipital neuralgia.
Symptoms of Arnold’s Syndrome (Occipital Neuralgia)
Occipital neuralgia often mimics the symptoms of a tension headache or migraine, which can make diagnosis challenging. The symptoms can vary from person to person, but the hallmark signs of Arnold’s Syndrome include:
Key Symptoms to Look For:
- Severe, sharp, or stabbing pain in the back of the head, neck, or behind the eyes
- Pain that worsens with neck movement or pressure on the scalp
- Tenderness in the scalp or neck, often along the occipital nerve pathway
- Pain that radiates to the forehead, temples, or behind the eyes
- Numbness or tingling sensations along the neck or scalp
- Sensitivity to light or sound (in some cases)
Pain is usually unilateral (on one side of the head) but can occur bilaterally (on both sides). The attacks may last for seconds or minutes but can come in waves, making daily activities difficult.
Diagnosing Arnold’s Syndrome (Occipital Neuralgia)
A proper diagnosis is essential to differentiate occipital neuralgia from other similar conditions, such as migraines or cluster headaches.
Steps in the Diagnostic Process:
- Medical History: Your doctor will ask about your symptoms, including the duration, intensity, and frequency of pain, as well as any history of neck injuries or trauma.
- Physical Examination: The doctor will examine your neck and head, pressing gently to check for tenderness and signs of muscle tension along the occipital nerve path.
- Imaging Tests: X-rays, MRI scans, or CT scans may be used to rule out other conditions, such as herniated discs, tumors, or other spinal issues that may be pressing on the nerves.
- Nerve Blocks: In some cases, a nerve block may be performed, where a local anesthetic is injected near the occipital nerve. If the pain is relieved, it confirms occipital neuralgia as the diagnosis.
Treatment Options for Arnold’s Syndrome (Occipital Neuralgia)
The treatment for occipital neuralgia typically involves a combination of medication, physical therapy, and, in some cases, surgical intervention. The goal is to reduce nerve inflammation, alleviate pain, and address any underlying causes.
1. Medications
- Pain Relievers: Over-the-counter pain medications like ibuprofen or acetaminophen can provide relief for mild cases. For more severe pain, prescription medications such as opioids or stronger analgesics may be used.
- Muscle Relaxants: These can help relax the neck muscles and reduce tension that may be irritating the occipital nerves.
- Anticonvulsants or Antidepressants: Medications like gabapentin (Neurontin) or amitriptyline may be prescribed to help manage nerve pain.
- Steroid Injections: Corticosteroid injections around the occipital nerve can help reduce inflammation and provide longer-lasting relief.
- Nerve Blocks: A local anesthetic or steroid is injected directly into the affected nerve to block pain signals and reduce inflammation.
2. Physical Therapy
Physical therapy can help alleviate neck tension and improve posture, reducing pressure on the occipital nerves. Techniques such as gentle stretching, massage, and strengthening exercises for the neck and upper back are common methods.
3. Surgical Treatment
In rare cases where conservative treatments don’t work, surgery may be considered. Surgical options include:
- Occipital Nerve Stimulation: A small device is implanted to deliver electrical pulses to the occipital nerves, helping to block pain signals.
- Nerve Decompression Surgery: In cases where nerve compression is severe, surgical decompression may be performed to relieve pressure on the occipital nerve.
Lifestyle Changes to Manage Arnold’s Syndrome (Occipital Neuralgia)
While medical treatment is essential, there are several lifestyle changes you can make to help manage the condition and prevent flare-ups.
Tips for Managing Occipital Neuralgia:
- Maintain Good Posture: Avoid slouching and keep your head in a neutral position to prevent strain on your neck and occipital nerves.
- Avoid Stress: High stress can exacerbate muscle tension and trigger pain. Relaxation techniques like meditation, deep breathing, or yoga can be beneficial.
- Heat or Cold Therapy: Applying a warm compress or cold pack to the affected area can provide temporary relief from pain and inflammation.
- Limit Neck Strain: Avoid activities that require extended neck movement, such as reading or using devices for long periods. Take regular breaks to stretch your neck.
When to Seek Medical Help
If you experience any of the following, it is important to seek medical attention promptly:
- Pain that doesn’t respond to over-the-counter medications
- Severe or worsening headache symptoms
- Symptoms that interfere with daily activities
- Numbness or weakness in the arms or legs
Conclusion
Arnold’s Syndrome (occipital neuralgia) is a painful condition that affects the occipital nerves, causing sharp, stabbing pain at the base of the skull, neck, and sometimes the forehead. Understanding the causes, symptoms, and treatment options is essential for managing the condition and improving quality of life.
With a combination of medication, physical therapy, and lifestyle changes, most individuals with occipital neuralgia can manage their symptoms effectively. Early diagnosis and treatment are key to preventing long-term nerve damage and alleviating pain.
If you or someone you know is experiencing symptoms of Arnold’s Syndrome, consult with a healthcare provider to receive the proper diagnosis and treatment.
Important Disclaimer: This article is for informational purposes only and should not replace professional medical advice. For health-related concerns, consult healthcare providers. Individual results may vary, and personal circumstances should always be considered when implementing any suggestions.