Meta Description: Explore COPD pathophysiology and symptoms. Learn how persistent airflow limitation develops, key clinical features, causes, and disease progression explained simply.
Chronic Obstructive Pulmonary Disease (COPD) is a long-term respiratory condition characterized by persistent airflow limitation that makes breathing progressively more difficult. It is not a single disease but a group of conditions—mainly chronic bronchitis and emphysema—that damage the lungs over time.
Understanding COPD pathophysiology and symptom progression is essential for recognizing early warning signs, slowing disease progression, and improving quality of life.
In this article, you’ll discover how COPD develops in the lungs, what causes airflow obstruction, and the key clinical symptoms that define the disease.
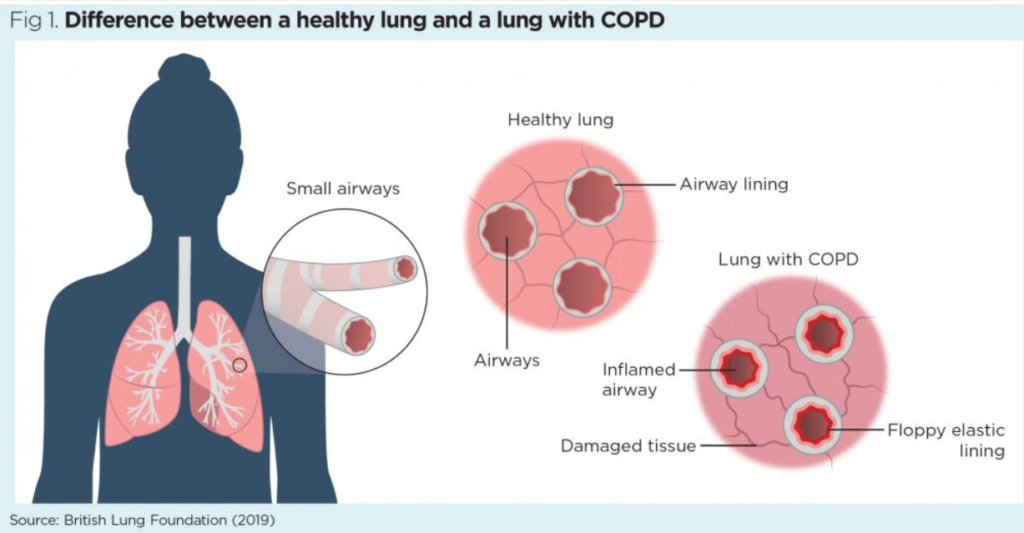
Understanding COPD and Its Impact on the Lungs
COPD primarily affects the airways and alveoli (air sacs) in the lungs, leading to reduced airflow and impaired gas exchange.
What happens in COPD?
- Airway inflammation
- Narrowing of bronchial tubes
- Destruction of alveolar walls
- Mucus overproduction
Why airflow becomes limited
The combination of inflammation, mucus buildup, and structural lung damage causes air to become trapped, making exhalation especially difficult.
Featured Snippet: What is the pathophysiology of COPD?
The pathophysiology of COPD involves chronic inflammation of the airways, destruction of alveoli, mucus hypersecretion, and narrowing of air passages, leading to persistent airflow limitation and impaired gas exchange.
Major Causes and Risk Factors of COPD
COPD develops gradually, often due to long-term exposure to harmful irritants.
1. Smoking (primary cause)
- Tobacco smoke damages airway lining
- Triggers chronic inflammation
- Accelerates lung tissue destruction
2. Environmental exposure
- Air pollution
- Occupational dust and chemicals
- Biomass fuel smoke
3. Genetic factors
A rare condition called alpha-1 antitrypsin deficiency can increase risk.
COPD Pathophysiology: What Happens in the Lungs?
1. Chronic airway inflammation
Inflammation is the core mechanism behind COPD progression.
What occurs:
- Swelling of airway walls
- Increased immune cell activity
- Thickening of bronchial lining
2. Mucus hypersecretion
Goblet cells produce excess mucus.
Effects include:
- Blocked airways
- Chronic cough
- Increased infection risk
3. Alveolar destruction (emphysema)
The alveoli lose elasticity and structure.
Consequences:
- Reduced oxygen exchange
- Air trapping in lungs
- Shortness of breath
4. Airflow obstruction
All these changes lead to:
- Narrowed airways
- Difficulty exhaling air
- Progressive breathing limitation
Featured Snippet: What are the main symptoms of COPD?
The main symptoms of COPD include chronic cough, shortness of breath (dyspnea), wheezing, chest tightness, increased mucus production, and fatigue, often worsening over time.
Clinical Features and Symptoms of COPD
1. Chronic cough
Often the earliest symptom.
Characteristics:
- Persistent
- May produce mucus
- Worse in the morning
2. Dyspnea (shortness of breath)
One of the hallmark symptoms.
Progression:
- Initially occurs during exertion
- Later present even at rest
3. Wheezing
- High-pitched breathing sound
- Caused by narrowed airways
4. Excess mucus production
- Thick sputum
- Frequent throat clearing
- Chronic bronchitis component
5. Fatigue and reduced exercise tolerance
Due to reduced oxygen delivery to tissues.
Step-by-Step: How COPD Progresses Over Time
Step 1: Early stage
- Mild cough
- Occasional breathlessness
Step 2: Moderate stage
- Increased mucus
- Noticeable airflow limitation
- Reduced activity tolerance
Step 3: Severe stage
- Frequent exacerbations
- Significant breathlessness
- Reduced quality of life
Step 4: Very severe stage
- Severe oxygen impairment
- Possible respiratory failure risk
Advanced Insights into COPD Mechanisms
1. Oxidative stress
Toxins from smoking increase free radical damage in lung tissue.
2. Structural lung changes
- Loss of elasticity
- Airway collapse during exhalation
3. Impaired immune response
Makes lungs more vulnerable to infections.
Common COPD Exacerbation Triggers
Respiratory infections
- Viral or bacterial infections often worsen symptoms
Air pollution
- Can trigger acute flare-ups
Cold weather
- May increase airway sensitivity
Smoking exposure
- Even passive smoke worsens symptoms
Internal Linking Opportunities
This topic connects well with:
- Respiratory system anatomy and function
- Smoking and lung disease prevention
- Oxygen transport in the human body
- Chronic inflammation and systemic disease
- Pulmonary rehabilitation and breathing exercises
Conclusion
Understanding COPD pathophysiology and symptom progression reveals how persistent airway inflammation, mucus buildup, and alveolar damage gradually restrict airflow and impair breathing. These changes explain why symptoms like chronic cough and shortness of breath worsen over time.
While COPD is a progressive condition, early awareness and lifestyle changes can help slow its progression and improve quality of life. Recognizing symptoms early and understanding the underlying mechanisms empowers better management and informed healthcare decisions.
By staying informed and proactive, individuals can take meaningful steps toward protecting lung function and maintaining better respiratory health over time.