Meta Description: Learn the differences in IBD pathology between Crohn’s disease and ulcerative colitis. Understand symptoms, inflammation patterns, and key clinical distinctions.
Inflammatory Bowel Disease (IBD) is a chronic group of disorders that cause long-term inflammation of the digestive tract. The two main types—Crohn’s disease and ulcerative colitis—are often confused, but they differ significantly in how they affect the gut.
Understanding the differences in IBD pathology is essential for accurate diagnosis, effective treatment, and better long-term disease management. While both conditions share symptoms like abdominal pain and diarrhea, their underlying patterns of inflammation are not the same.
In this article, you’ll learn how Crohn’s disease and ulcerative colitis differ in location, depth of inflammation, symptoms, and complications.
What is Inflammatory Bowel Disease (IBD)?
IBD refers to chronic inflammation of the gastrointestinal tract caused by an abnormal immune response.
Main types of IBD
- Crohn’s disease
- Ulcerative colitis
Why IBD develops
The exact cause is not fully understood, but it involves:
- Immune system dysfunction
- Genetic predisposition
- Environmental triggers
- Gut microbiome imbalance
Featured Snippet: What is the difference between Crohn’s disease and ulcerative colitis?
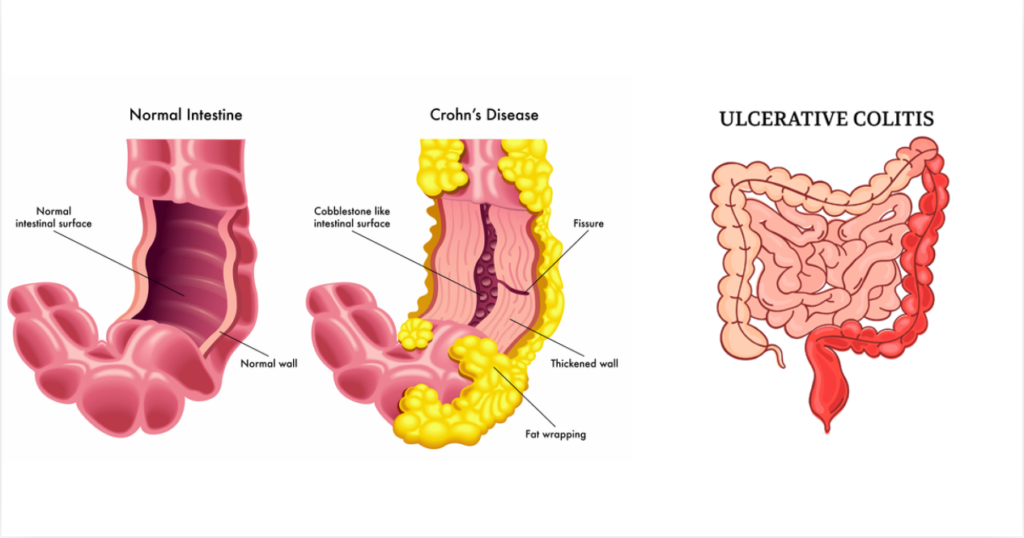
Crohn’s disease can affect any part of the gastrointestinal tract and causes patchy, deep inflammation, while ulcerative colitis affects only the colon and rectum with continuous, superficial inflammation of the intestinal lining.
Crohn’s Disease: Pathology and Characteristics
Crohn’s disease can affect any part of the digestive tract—from mouth to anus.
1. Location of inflammation
- Can occur anywhere in the GI tract
- Most common in the terminal ileum and colon
2. Pattern of inflammation
- “Skip lesions” (patchy areas of inflammation)
- Affects all layers of the intestinal wall (transmural inflammation)
3. Key pathological features
- Thickened bowel wall
- Ulcers and fissures
- Granuloma formation (in some cases)
4. Common symptoms
- Abdominal pain
- Chronic diarrhea
- Weight loss
- Fatigue
Ulcerative Colitis: Pathology and Characteristics
Ulcerative colitis is limited to the colon and rectum.
1. Location of inflammation
- Affects only the large intestine
- Always begins in the rectum and spreads upward continuously
2. Pattern of inflammation
- Continuous inflammation (no skip lesions)
- Affects only the inner lining (mucosa and submucosa)
3. Key pathological features
- Ulceration of the colon lining
- Pseudopolyps formation
- Mucosal bleeding
4. Common symptoms
- Bloody diarrhea
- Urgency to defecate
- Abdominal cramps
- Fatigue
Key Differences in IBD Pathology
1. Location of disease
- Crohn’s disease: anywhere in GI tract
- Ulcerative colitis: only colon and rectum
2. Depth of inflammation
- Crohn’s: full thickness (transmural)
- UC: superficial layers only
3. Pattern of lesions
- Crohn’s: patchy (skip lesions)
- UC: continuous inflammation
4. Presence of blood in stool
- Crohn’s: less common
- UC: very common
Featured Question: Why is Crohn’s disease more complex than ulcerative colitis?
Crohn’s disease is more complex because it can affect multiple areas of the digestive tract in patchy patterns and involves deeper layers of the bowel wall, leading to complications like strictures, fistulas, and abscesses.
Complications of Crohn’s Disease
Because it affects deeper layers, Crohn’s can lead to:
- Bowel strictures (narrowing)
- Fistulas (abnormal connections)
- Abscesses
- Malnutrition
Complications of Ulcerative Colitis
Since UC is limited to the colon:
- Severe bleeding
- Toxic megacolon
- Increased risk of colon cancer
Diagnosis of IBD
Doctors use a combination of tests:
- Colonoscopy
- Biopsy
- Blood tests (inflammation markers)
- Imaging (CT or MRI scans)
Step-by-Step: How IBD is Differentiated Clinically
Step 1: Evaluate symptoms
- Bloody stool suggests UC
- Patchy pain suggests Crohn’s
Step 2: Perform endoscopy
- Continuous inflammation → UC
- Skip lesions → Crohn’s
Step 3: Confirm with biopsy
- Tissue depth and immune patterns confirm diagnosis
Advanced Insights into IBD Pathology
1. Immune system dysfunction
IBD is driven by an overactive immune response attacking gut tissue.
2. Role of gut microbiome
Imbalance in gut bacteria may trigger inflammation.
3. Genetic influence
Certain genes increase susceptibility to both conditions.
Lifestyle Factors Affecting IBD
While not a cause, lifestyle can influence flare-ups:
- Stress levels
- Diet quality
- Smoking (worsens Crohn’s)
- Sleep patterns
Internal Linking Opportunities
This topic connects well with:
- Digestive system inflammation and gut health
- Immune system disorders
- Colon health and digestive diseases
- Nutrition for inflammatory conditions
- Microbiome and gut balance
Conclusion
Understanding the differences in IBD pathology between Crohn’s disease and ulcerative colitis is essential for recognizing symptoms, supporting early diagnosis, and managing long-term health. While both conditions involve chronic intestinal inflammation, they differ in location, depth, and pattern of damage.
Crohn’s disease can affect any part of the digestive tract and penetrates deeply, while ulcerative colitis is limited to the colon and causes continuous superficial inflammation. These differences guide diagnosis and treatment strategies.
With proper medical care, lifestyle management, and awareness, individuals with IBD can achieve better symptom control and improved quality of life.